Knee pain
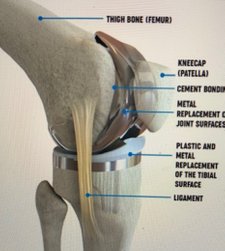
Total Knee Replacement
Description
This surgery is a replacement of a damaged or worn knee joint with an artificial metal joint. The medical term for this type of surgery is 'arthroplasty'. Knee replacement surgery (arthroplasty) aims to relieve knee pain and improve joint movement. It take two hours, you needs three onths to fully recover.
Excpect
After the operation your knee will be swollen for 6-8 weeks, pain will never go to zero, some skin numbness on the outside of the scar which will get smaller with time, some clicks and noises can arrive from the new knee.
Complications
All surgery carries a slight degree of risk. However, most people do not have any complications. Knee replacement surgery (arthroplasty) is now a routine and commonly performed operation in the UK.
Someone who is fit and with no other medical problems will be at a lower risk than a person with multiple medical conditions.
Evidence indicates that the risks of complications are reduced, and patient satisfaction with the outcome is increased, if the surgeon is familiar with the procedure.
Your anaesthetist and surgeon will be able to answer any questions you may have about your personal risks from anaesthetics and the surgery itself. Complications like, infection (deep or superficial), pain, swolling, DVT, wound healing, bleeding, fractures, loosing of the prosthesis with time.
Partial Knee Replacement
Description
This procedure is much less invasive than total knee replacement and may give relief to people suffering from arthritis of the knee or a knee injury. Partial knee replacement surgery replaces only the damaged area of your knee joint, may require only one or two days of hospitalization, and results in a shorter recovery time when compared with total knee replacement surgery.
The knee can be divided into three compartments: the medial compartment - the inside part of your knee, the lateral compartment - the outside part of your knee, and the patello-femoral compartment - the area where your kneecap rests. The unicompartmental implant is designed to replace either the media (inside) or lateral (outside) compartment.
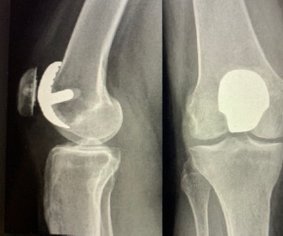
The X-ray below left shows a right leg with a degenerated medial (inside) compartment. Notice how there is no space between the femur (thigh) bone and tibia (shin) bone. This bone on bone contact can be quite painful.
The Procedure
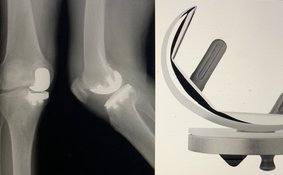
The partial knee replacement procedure begins with the exposure of the joint through a 3-4 inch incision. The surgeon then properly balances the knee joint. Next the surgeon shapes the end of the thigh bone (femur) and the top of the shin bone (tibia) to accommodate the unicompartmental knee replacement components. He places trial components on the bones to ensure proper alignment and removes them once this alignment is achieved. Finally, the surgeon implants the femoral and tibial components, closes the incision, and the procedure is complete.
Returning Home
You will be discharged when you can get out of bed on your own and walk with a walker or crutches, walk up and down three steps, bend your knee 90 degrees, and straighten your knee. You will continue your home exercise program and go to outpatient physical therapy, where you will work on an advanced strengthening program and such programs as stationary cycling, walking, and aquatic therapy.
Your long-term rehabilitation goals are a range of motion from 100-120 degrees of knee flexion, mild or no pain with walking or other functional activities, and independence in all activities of daily living.
Knee cap replacement
Description
A New and Better Way to Restore Knee Function and Relieve the Pain of Kneecap Arthritis, Wear pain and loss of function from kneecap (patella) arthritis and cartilage wear is a common problem afflicting up to 10 % of the population. Often patients undergo multiple operations only to end up with severe disability.This is because many of the traditional solutions have been shown to have fairly high failure rates averaging 30 %. In addition,establishing the correct cause of kneecap pain and knowing when to perform any one operation and as importantly knowing what operation not to do is critical to successful treatment.
Indication
Severe PFJ signs & symptoms.
Radiological evidence of PFJ O.A.
Failed re-alignment PFJ.
Failed patellectomy.
Arthroscopic finding of pure PFJ O.A.
Young patient with early O.A.
Post traumatic fracture patella.
Knee arthroscopy
Description
Under general anaesthesia, looking inside the knee joint via a telescope about as wide as a pen, connected to a television monitor.
The surgeon will insert the arthroscope tools through one or two tiny cuts (about half an inch 1.2cm) around your knee. This operation called knee arthroscopy. If you have torn a cartilage, the surgeon will remove the torn part using fine instruments inserted through small cuts. Occasionally he has to make a bigger cut to remove the cartilage. This would be about three inches (7.2cm) long.
If you have torn a ligament within the knee, he will not replace it during this operation. He will discuss the possible treatments with you after your arthroscopy. If he finds a loose bone fragment, he will remove it through the small cuts. If you have arthritis, he can see how severe it is. He will wash out the knee with salt water. This often improves your symptoms for some months. The cuts will be closed with paper tapes or stitches.
The operation can either be done as a day case, which means that you come into hospital on the day of the operation and go home the same day, or as an inpatient case, which means spending one night in hospital. Your surgeon will discuss with you which way you will be having the operation.